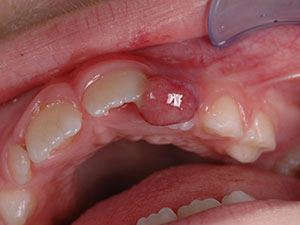
Epulis
Orofacial granulomatosis and epulis
AimThe rare diseases orofacial granulomatosis (OFG) and epulis represent two separate clinical entities, both with uncertain aetiologies and clinical features. Despite a number of case reports and reviews in previous years, these illnesses still pose a medical challenge. The aim of this literature review is to summarize the most essential pieces of information for both illnesses and provide an overview of the literature from recent years up until August 2015. Strived to be answered are these main questions: What is the momentary knowledge of orofacial granulomatosis and epulis? What is known about their aetiology, prevalence, clinical and histological findings and therapy? Are there any synonyms for the same clinical pathology and are there any overlapping names with a different clinical meaning?
Introduction
Because of the various synonyms and diffuse medical terms, no all-round agreement between clinicians exists regarding the characterization of the diseases and the classification of the possible subtypes. At present, in medical journals and online databases, such as PubMed, there are existing reviews and case reports about orofacial granulomatosis and epulis. However, compared to well-known diseases, studies of these illnesses are rare and accordingly, knowledge is sparse and spread out across the available literature. There are still gaps where precise data is missing and the diagnosis and treatment of these two illnesses therefore remain a challenge.
Methods
The literature research for this review includes three different methods of proceeding: textbooks, E- Journals and online databases such as PubMed, so as to provide a widespread selection of the different reports available.
Summary of the main characteristics
Orofacial granulomatosis (OFG)
Orofacial granulomatosis (OFG) describes a rare illness, characterized by sub- epithelial granulomas which appear not only in the oral cavity, but also in the soft tissue of the face. 5,6 There are various synonyms and differential terms such as Melkersson- Rosenthal syndrome, oral Crohn's disease and cheilitis granulomatosa. 7 Other similar clinical presentations are seen in illnesses such as sarcoidosis, tuberculosis, leprosy, syphilis and sometimes even fungal infections. 7,24 The aetiology of orofacial granulomatosis is essentially uncertain, however, there are multifactorial hypotheses regarding possible triggers, such as allergic, infectious (e.g. S. aureus), idiopathic or even genetic factors (higher levels of HLA). 5,11 OFG patients seem to be more frequently affected by food sensitivities and therefore should be tested. 8 Results from past studies have suggested that patients with OFG might be in an immunodeficient state. 27 OFG normally appears in young adults as well as adolescents and there seems to be no sex or race predilection. 2,7,22 Unfortunately, the exact prevalence in children still remains unknown. 18 Overall, the incidence of OFG appears to be increasing. 23 The typical clinical presentation of OFG is recurrent and later on a persistent, non- pruritic, firm and non- tender i.e. painless lip or facial swelling. 2,4,5,6 Three main types of swelling have been observed: recurrent, progressive and persistent. 19 The changes in the mucosa can be or present: hyperplastic, ulcerating, erythema, mucosal tags, papules, cobblestone appearance. 3,5,7 Alarmingly, the orofacial swelling becomes permanent after several relapses and therefore damages the soft tissues and results in aesthetic impairment of the facial appearance. 23 Histologically, OFG often presents an unspecific, chronic inflammation alongside Langerhans- giant cells and non- caseating epitheliod cell granulomas 5 in the lamina propria, which then can cause an obstruction of the lymphatic vessels leading to these clinical swellings. 26 OFG is stated to be a type of delayed hypersensitivity reaction, without knowing which specific antigen has caused it. The causative antigen seems to vary in each patient. 26 There are various ways to diagnose OFG, for example, biopsy or patch tests. 5,7,10 Differential diagnoses are, for example, Crohn's disease, perianal disease, sarcoidosis, tuberculosis and syphilis. 7,18,24 Up until now, no ideal treatment has been found which promises complete recovery for every patient without any recurrences. Accordingly, treatment for orofacial granulomatosis remains symptomatic. (E.g. corticosteroids) 5,7 Early diagnosis of OFG is extremely important, since the end results of the therapy prove to be much better. 5 Clinicians have to be aware of the fact that symptoms in OFG patients are multiform and can change in the course of the disease. 1
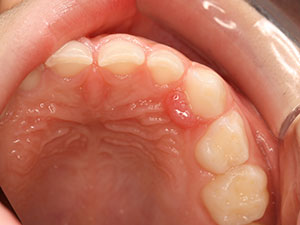
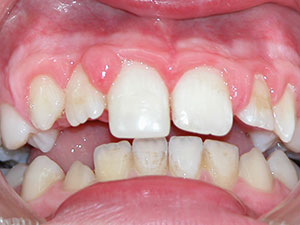
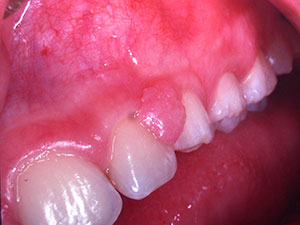
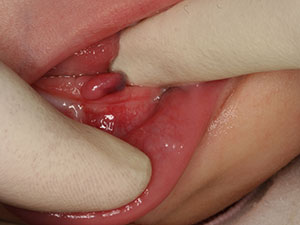
Epulis
The term epulis is defined as a hyperplastic gingival tissue or a gingival tumour mass. 31 From the articles selected, it was possible to classify epulis into five main categories: congenital epulis (CE), congenital fibrous epulis (CFE), pyogenic granuloma (PG), fibrous epulis (FE) and peripheral giant- cell granuloma (PGCG). 13,29 The many synonyms and differential terms result in a lack of consensus and, therefore, the diagnosis of the epulides remains a challenge. There is a large spectrum of possible aetiologies leading to epulides, ranging from odontogenic origins, small tissue traumas, bacterial infections, bad oral hygiene, faulty restorations to repetitive gingival irritants. 9,12,13,17,29 The prevalence of epulides varies depending on the type of epulis. Therefore, epulides can be present at birth, or appear later on in life (PG, FE, PGCG). 13,17,29 The sex predilection also depends on the type of epulis in question. The predilection sites also differ, but mainly the alveolar mucosa of the maxilla is affected and can reach up to 90mm in size. 13,16,17 Unfortunately, it is possible that some types of epulides show recurrences and can even become malignant. 25 Epulides can be sessile, freely mobile or pedunculated, show ulceration and the colour can range from pink to reddish or even blue or brown. 12,13,14,16,21,29 As mentioned above, there is no sole way of diagnosing the different types of epulis. Some methods used are: MRI, 2- or 3- dimensional ultrasonography, histological analyses, Doppler ultrasound or biopsies. 20,30 Spontaneous remission can occur depending on the epulis but if not, therapies such as excision, lasers, elimination of possible irritants, cryosurgery or intralesional injections are required. 14,15,28 It is of great importance to recognize these various forms of epulis to facilitate the required treatment as quickly as possible. 30
Conclusion
Despite OFG and epulis becoming better known to clinicians, they are still a challenge to diagnose, due to the multiple clinical features and differential diagnoses. The number of various synonyms and differential terms complicate recognition and understanding of the illnesses. There is a significant need for standardization and further classification of the two terms OFG and epulis. By conducting studies on a larger scale, additional research into perfecting the necessary therapies could be achieved and is thus of interest and importance for the future. A worldwide online databank is of great use to raise further awareness of these rare illnesses and to gather much needed data. back